4th shots of Pfizer, Moderna vaccines provide near equal protection — Israeli study
Sheba-led research team says that 6 months after boosters, ‘antibody levels and cumulative vaccine efficacy do not differ between the two vaccines’
Nathan Jeffay is The Times of Israel's health and science correspondent
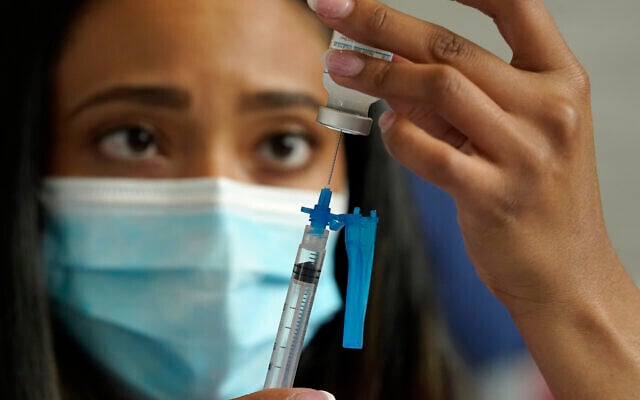
Booster shots developed by Pfizer and Moderna provide near equal protection against COVID-19, according to Israeli research.
The newly peer-reviewed study on fourth shots could help reduce anxieties felt by some over whether they are receiving the best vaccines, with the authors concluding that for the most part people should take what is available.
“Differences were very subtle and choices can be shaped by logistical concerns over efficacy,” Dr. Noam Barda of Sheba Medical Center and Ben Gurion University, one of the researchers, told The Times of Israel.
“As far as immune response and effectiveness, this indicates both as a fourth shot are similar.”
The Sheba-led research team, headed by Barda and Dr. Michal Canetti, acknowledged two limitations to their study: It only covered 274 people, who are healthcare workers and thus do not represent a full-cross section of society in terms of age.
They also noted the study — which was conducted between December and July — relied on regular vaccines that most of the world is still using, to administer the fourth doses, and not the newly released shots that have been bolstered to fight variants. Israel began administering the Omicron-specific vaccines last month.
The researchers monitored Sheba workers, some of whom received the Moderna vaccine as a fourth shot and others who had received the Pfizer vaccine.
All the participants had initially received three Pfizer shots but had low antibodies at the time of their booster. None had knowingly been infected with COVID-19.
“In this study, we observed that six months-post-fourth dose, antibody levels and cumulative vaccine efficacy do not differ between the two vaccines,” the researchers wrote.
Their findings “suggest that choosing with which of the two vaccines to provide booster doses should depend mostly on availability.”
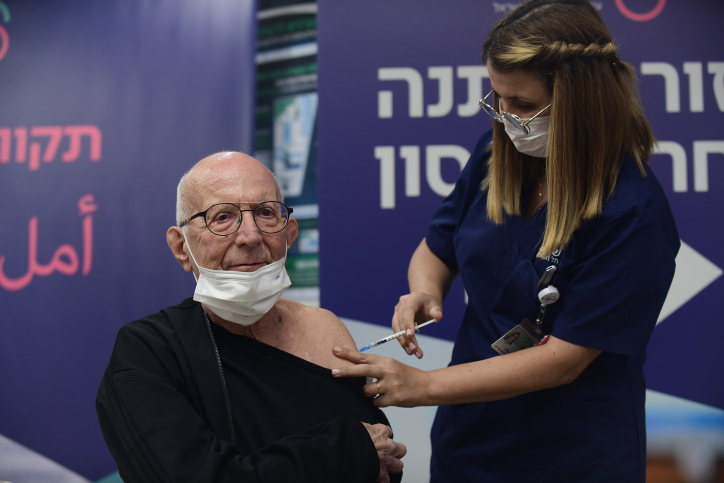
During the half-year period of the study, which started in December and covered Israel’s Omicron wave, 58.3 percent of Moderna and 57.8% of Pfizer recipients were infected.
Moderna recipients had a slightly lower propensity for “substantial” disease which was defined as spending two or more days in bed: 6.5% versus 10%. However, as only 21 people across both groups fell into this category, the authors considered this as a “minor, non-significant advantage.”
Addressing the limitations of the study, the authors wrote that the small sample size “does not allow us to assess the less common more severe outcomes, for example, hospitalization and death.”
The other weakness, which they called “the issue of generalizability,” relates to whether a sample of healthcare workers can provide valuable insight given that few are elderly.
Answering this, the researchers stressed the study included hospital volunteers, many above the retirement age. The mean age of participants in the study was 58.
The Times of Israel Community.











