As more troops survive injuries, some credit battlefield transfusions of whole blood
IDF only military in the world currently performing procedure pioneered by US army; while no proof yet to declare it a panacea, fight against Hezbollah may prove its worth
Renee Ghert-Zand is the health reporter and a feature writer for The Times of Israel.

In the Second Lebanon War, 14.9 percent of wounded IDF soldiers died from their injuries. In Operation Protective Edge in 2014, the percentage decreased to 9.4%. In the current war, only around 7% of those wounded in battle have died.
The IDF Medical Corps and physicians who treat the war-wounded in Israel’s hospitals cite several reasons for the historically low case fatality rate — the ratio of injured who survive to the number of injured who die.
Among those reasons is the rapid evacuation time by helicopter, which on average get the injured to a hospital trauma room in just over an hour. Also noted is the high number of senior-level medical personnel, including physicians and paramedics, on the battlefield. Each company has a medical professional in the field with it, who reaches a wounded soldier within five to seven minutes.
The final factor is the military’s decision to give whole blood transfusions on the battlefield for the first time. This is possible because qualified medical personnel are right there to do it.
“This is something happening only in the Israeli military and it’s an amazing game changer,” said Col. Zivan Aviad-Beer, chief medical officer of the IDF Southern Command, speaking to the Hebrew-language Haaretz in December.
“What a wounded person is missing is not fluids, but blood. Blood carries oxygen and provides clotting factors,” he explained.
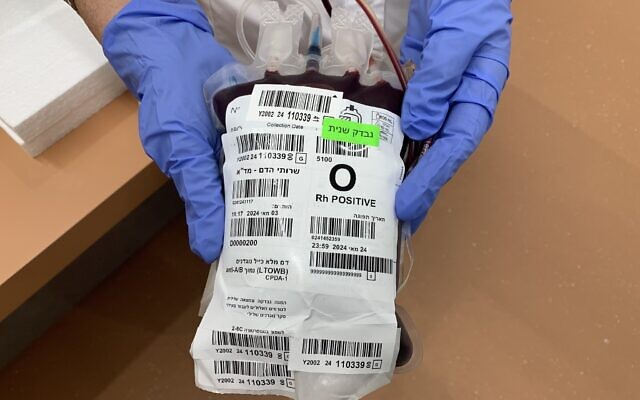
Is whole blood the answer?
When a soldier is wounded on the battlefield, the most important thing to do is to stop the bleeding as quickly as possible, Dr. Yoram Klein, director of trauma at Sheba Medical Center, told The Times of Israel.
This is achievable by various methods, including tourniquet, compression and packing of a wound if it is external, such as an amputated limb or shrapnel in the thigh.
However, internal bleeding can only be stopped by surgery. Giving a wounded soldier whole blood in the field can extend the time they can stay alive until reaching a hospital.
It’s impossible to ascribe the low-case fatality rate to the transfusions alone, as the beneficial effects of whole blood transfusions while still on a battlefield have yet to be scientifically proven, though anecdotal evidence exists.
“The theory and logic are there, but to answer scientifically whether this is beneficial you need to conduct a randomized study comparing the results for wounded soldiers who got the whole blood [in the field] versus those who did not. Conducting such a study would not be easy,” Klein said.
“You also need to isolate the effect because giving whole blood was not the only thing that they did in the field. Undoubtedly, the most significant achievement of the IDF Medical Corps has been the speed of the evacuations,” he said.

“In the war in Gaza, we were lucky that the front was close to a handful of major trauma centers. In the case of a war on the northern border with Lebanon, that would not be the case. The evacuation distances would be greater,” Klein said.
Whole blood: What’s old is new again
Originally, all blood transfusions were whole blood. It was only in the middle of the 20th century that donated blood units began being separated into components: red blood cells (packed cells), plasma, platelets and cryo. Each must be stored at different temperatures and has a different shelf life.
According to Klein, the change occurred as a way of making the most of donated blood, as most transfusions are given to sick patients who need a specific blood component rather than all of the blood.
Prof. Eilat Shinar, director of the Magen David Adom National Blood Services, told The Times of Israel that only 10% of the blood it collects and processes goes to the IDF. Klein said that even during the war, most of the blood supply at Sheba is used for patients other than wounded soldiers.

Historically, MDA gave the IDF’s Unit 669, which specializes in aerial rescue missions, concentrated red blood cells for use wherever needed. Elite IDF units also carried units with them.
The idea of giving whole blood cropped up in the early 2000s when US forces in Iraq and Afghanistan found themselves having to treat wounded troops in remote areas far from military bases and field hospitals. When necessary, they simply drew a unit of whole blood from one soldier in the field and gave it to a wounded one.
“It worked. Why wouldn’t it? [The wounded soldier] loses everything and gets back everything,” Shinar said.
According to Shinar, civilian rescue helicopter crews in Norway that serve remote regions and have long evacuation times have adopted the use of whole blood. The US military is also using it, but not on the battlefield.
“The IDF is the only one using it right on the front lines,” she emphasized.
Shinar said that using whole blood, either in the field or in rescue helicopters or ambulances, makes it much easier for medical crews. Instead of dealing with multiple bags and lines for saline, red blood cells and freeze-dried plasma in tight quarters, there is just one bag to handle.
Making whole blood safe for every recipient
Like all donated blood, the whole blood units MDA prepares for the IDF and others are tested for blood type and blood-borne diseases. In contrast, they do not undergo the component separation process and they are all blood type O-positive. O-negative blood is considered the universal donor type, but O-positive is given in emergencies in Israel because 85% of Israelis are Rh-positive, meaning they can be compatible for other positive blood types.
“It’s okay if someone who is Rh-negative gets one transfusion of O-positive blood. If there is a problem, it can be dealt with at the hospital,” Shinar explained.

MDA sends the whole blood units out to the army in small, portable coolers. Whole blood can theoretically be stored for 35 days, but MDA has the army return any that is not used within 21 days and sends fresh supplies out to ensure quality.
Shinar said that once a wounded patient arrives at the trauma room, tests are done to determine what blood component they need from that point on. However, Klein said that whole blood is often used nonetheless in the trauma room, as it is simple and convenient.

“I am glad that they are using a lot of whole blood in this war. I am not sure it made a huge difference in the outcomes for wounded soldiers, but the IDF medical personnel have learned how to use it. This could be critical for what may come,” Klein said.
“On the Lebanese front, the evacuations will not be as quick and the situation may be completely different. Then whole blood transfusions might really be the difference between life and death,” he said.
The Times of Israel Community.











