Israeli scientist leads search for Ebola cure
BGU virologist Dr. Leslie Lobel is developing a vaccine by studying the immune systems of the disease’s survivors
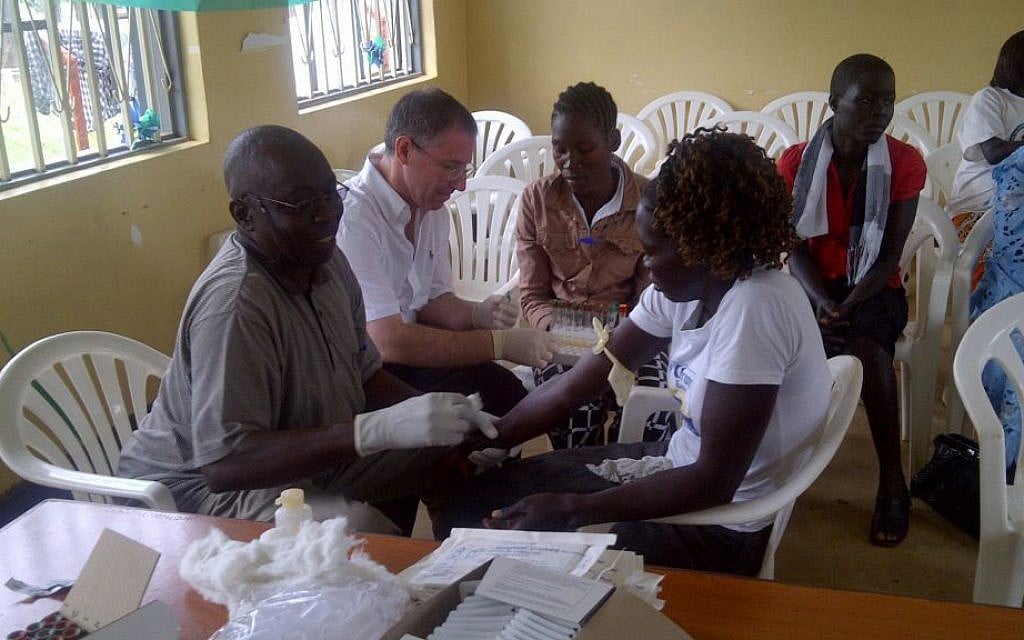
Unlike many people, Dr. Leslie Lobel has not been shocked to hear about the current Ebola epidemic in West Africa, the largest ever recorded since the virus’s discovery in 1976 in the Democratic Republic of the Congo (then Zaire). A Ben-Gurion University of the Negev virologist and a leader in the search for a cure for the devastating disease, Lobel had been predicting such an outbreak.
The quick spread this time of the disease in Sierra Leone, Liberia, Guinea and Nigeria has demonstrated the dire need for the vaccine that Lobel and his team have been working toward for the past 12 years by researching the natural immune system of Ebola survivors in Uganda.
The virus spreads from person to person through direct contact with bodily fluids. Individuals infected with Ebola usually begin to show symptoms of the disease eight to 10 days after exposure to the virus. Initial symptoms are similar to those of the flu, but in about half of cases, the person begins to hemorrhage. Soon, blood vessels deep inside the body begin to leak fluid. This leads to extremely low blood pressure that causes damage to internal organs. In previous outbreaks, between 60 and 90 percent of cases were fatal.
“This outbreak is really just a progression of what has been happening,” Lobel said of the epidemic, which has so far killed more than 1,600 people since March.
“It is a result of the fact that the world has fallen asleep when it comes to fighting infectious diseases. There has not been enough surveillance or development of expertise to control infectious diseases since the 1970s,” he said.

In addition, Lobel cited globalization and global warming as factors leading to the current outbreak of the hemorrhagic fever. Both have upset the ecological niches of bats, which many scientists believe serve as the reservoir for the virus.
It is believed that apes and humans become infected with Ebola after eating food that has been drooled or defecated on by bats, or by touching surfaces that have come in to contact with bat droppings and then rubbing their eyes or mouths.
“It has actually has not been proven that bats are guilty. It has been demonstrated that they are for Marburg [another hemorrhagic fever virus], but not for Ebola,” Lobel said.
“But bats are the likely reservoir. It makes sense because bats don’t fly far and don’t usually come into contact with people. This would explain the limited scope of Ebola outbreaks.”
Lobel, whose interest in Ebola was first piqued while he was at New York’s Columbia University before immigrating to Israel in 2002, has been traveling to East Africa five times a year for his research.
He and his co-principal investigator Dr. Victoria Yavelsky are partnering with the US military and the Uganda Virus Research Institute to devise a way of conferring long-term immunity against the disease through the use of human monoclonal antibodies.
The close collaboration with the US military on the study has been key, as the Ben-Gurion University scientists cannot work with the Ebola virus in Israel. There are very few high containment labs anywhere in the world, and there are none at Israeli universities.
“First of all, high containment labs are very expensive to operate. And second of all, there is the security issue here in the Middle East. Working with Ebola here is just asking for trouble,” Lobel said.
The team’s goal is to develop a passive vaccine composed of preformed components of the immune system, which would provide immediate protection against the virus.
“This would be much quicker than the active vaccine that the US military has already produced and shown effective in monkeys,” said Lobel. “An active vaccine takes about a month to take hold.”
(CNN reported this week that an experimental drug developed by the biotech firm Mapp Biopharmaceutical Inc. that had been tested on monkeys, but never before on humans, had been administered to an American missionary worker who became sick from Ebola in Liberia.)

Lobel has been following 120 Ugandan Ebola survivors, half of them since he began his research program more than a decade ago. It took the doctor a number of years to gain the trust of the survivors, who come from a culture in which people are very suspicious of medical professionals and some even blame doctors for the spread of the disease.
Setting up effective logistics and social work systems have been crucial to Lobel’s team’s work in Uganda.
“It really took me a while to change my philosophy of how to work with people. I work with local scientists and have learned to be very respectful,” Lobel said. “I spend a lot of time with each Ebola survivor.”
Whereas in the developed world, survivors of terrible diseases are seen as blessed, Ugandan survivors of Ebola are viewed as cursed by their countrymen.
“They feel like pariahs. Many of them have lost their jobs because they survived the disease,” Lobel said.
Lobel is keeping a close eye on the current outbreak, which is spreading faster than previous ones. He believes this is because of its location in West Africa, where the imposition of quarantines that would cause the disease to burn itself out are not being successfully imposed.
“This one is so bad because in the past the outbreaks were limited to Central Africa, where there is very good security. The police and army in those countries can control the movement of people,” the doctor said.
Unfortunately, Lobel’s research has not yielded a vaccine in time to help the victims of the current Ebola epidemic. However, the doctor believes that he and his team are just three to five years away from arriving at what he calls a “cocktail” consisting of a vaccine and a therapeutic that can be deployed as soon as an outbreak is detected.
“It’s going to happen, but there is nothing around the corner yet,” he said.

She died more than four decades ago, but Leah Goldberg remains a magnetic and enigmatic figure: Israel’s most beloved poet, a powerful woman who lived with her mother and never married, who reinvented herself from the ashes of World War I through her magical writing.
You can screen 'The Five Houses of Leah Goldberg' June 4-11. Join The Times of Israel Community today to support our work and watch this and other outstanding documentary films in our DocuNation series.

We’re really pleased that you’ve read X Times of Israel articles in the past month.
That’s why we started the Times of Israel - to provide discerning readers like you with must-read coverage of Israel and the Jewish world.
So now we have a request. Unlike other news outlets, we haven’t put up a paywall. But as the journalism we do is costly, we invite readers for whom The Times of Israel has become important to help support our work by joining The Times of Israel Community.
For as little as $6 a month you can help support our quality journalism while enjoying The Times of Israel AD-FREE, as well as accessing exclusive content available only to Times of Israel Community members.
Thank you,
David Horovitz, Founding Editor of The Times of Israel
The Times of Israel Community.









