Coronavirus pandemic is fast-tracking a health-tech revolution, expert says
The ‘floodgates are now open’ and regulators, patients and healthcare providers are all going with the flow, according to Yair Schindel of aMoon VC fund
Shoshanna Solomon was The Times of Israel's Startups and Business reporter

The coronavirus pandemic has fast tracked the merger of high tech with the health sector, leading to a health-tech revolution that will come about much faster than it would have otherwise, a venture capital fund expert said.
“We have a new normal,” said Yair Schindel, managing partner and co-founder of aMoon, a global HealthTech VC fund based in Israel, in an interview with The Times of Israel. “The world has changed dramatically,”
Schindel was part of a team of experts set up by the Health Ministry to develop guidelines on minimizing the impact of the coronavirus pandemic, which has killed over 377,000 people and infected over 6.3 million. In Israel the death toll from the virus has reached 289, with over 17,000 people infected.
Thanks to the virus, the timeline of the ongoing health-tech revolution has now shortened “quite dramatically,” he said. “We will see changes happening significantly faster than we originally anticipated.”

This revolution is now happening on a number of fronts, he explained, the first one being the patients themselves.
For many years everything that had to do with remote healthcare and telemedicine was difficult for many patients to accept, he said. They felt they needed the doctors to see them, to examine their lungs, their hearts, their throat.
“All these things today, in the mind of the patient, are no longer a necessity,” he said. Not only do patients today accept being treated from afar, they actually prefer it in order to avoid the risk of catching something at the doctor’s office.
Technologies that facilitate remote treatment have helped bridge this psychological gap for patients in general. “That is a huge step forward,” Schindel said.
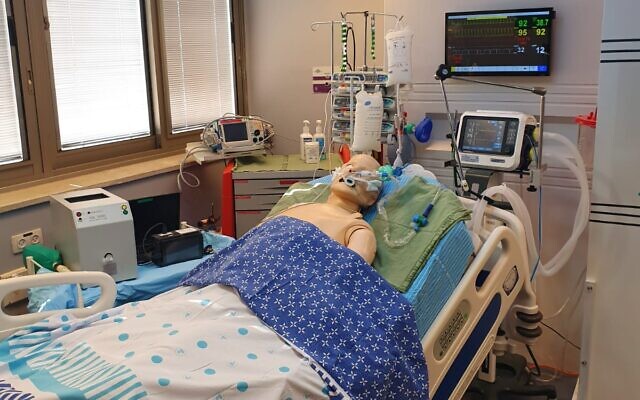
Earlier this month, Sheba Medical Center, at the forefront of Israel’s fight against COVID-19, unveiled what it called the “hospital of the future” – in which robots, AI and augmented reality do much of the work while doctors and nurses stay at a distance. Sheba has also utilized the Vici telemedicine system, a robot-like device that monitors patients’ vital signs.
Other systems include Tytocare, which allows physicians to remotely examine patients using stethoscopes, thermometers, and lung monitoring, and EarlySense, for the real-time delivery of actionable data along with patient data management tools that allow physicians to pinpoint and prevent potentially serious medical situations before they escalate.
Not only patients changed their frame of mind, said Schindel. Regulators, both in the US and Europe, “understand they have to move a lot faster,” he said.
“Obviously, we don’t want to put patients at risk, but if we can accelerate the process of approval for things that are safe and efficacious, we should do that as soon as possible,” he said. That is especially true for digital therapeutics, when software programs are used to prevent, manage or treat medical disorders, or when platforms are created to help analyze medical data and provide insights to physicians.
“For a while we didn’t know how fast it would go forward. Now it is basically a flood, and the floodgates are now open,” he said, referring to both technologies that are are being developed faster and regulatory approvals.

Healthcare providers, too, have realized they need to make more use of devices and technology to treat patients at home, rather sending them unnecessarily to already jam-packed hospitals.
Lastly, said Schindel, the genomics revolution that is taking place — what he calls the study of “the barcode with which we came into the world” — will further get a boost by the coronavirus pandemic.
“All the large pharma companies and academic institutions are trying to figure out who is influenced by COVID-19 and who isn’t,” he said. “Who will have a mild or more serious disease? Is it related to certain types of genes, or actually to certain types of proteins that some of us have or don’t?” All of these questions will help advance genomics research, he said.

Schindel, who was recruited by the director general of the Health Ministry to join the task force early in the crisis, said that he believes Israel deserves a “very high grade” in its effort to keep the virus at bay because it quickly took stringent steps, and because citizens are well versed in going into and out of emergency mode.
The ability to “quickly adapt and transition from routine day to day to emergency mode is a huge advantage of the Israeli people,” he said.
“Suppose we were not as responsive as we were; we would have ended up with numbers like some of these European countries,” he said. According to Statista, Israel has had 31.97 deaths per million inhabitants, compared to 821.92 per million in Belgium, 580.41 per million in Spain ,569.07 per million in the UK and 548.42 per million in Italy.
“Let’s say we knew there was a risk of some terror attack that could cause the loss of 3,000 lives and maybe another 20,000 injured or sick, via bioterror. What would the country do? Would we be willing to endure a month of lockup to avoid something like that? I think the answer is yes.”
Israel has eased lockdown measures as the virus spread slowed, but a resurgence of infections has raised the specter of renewed restrictions.
The Times of Israel Community.











